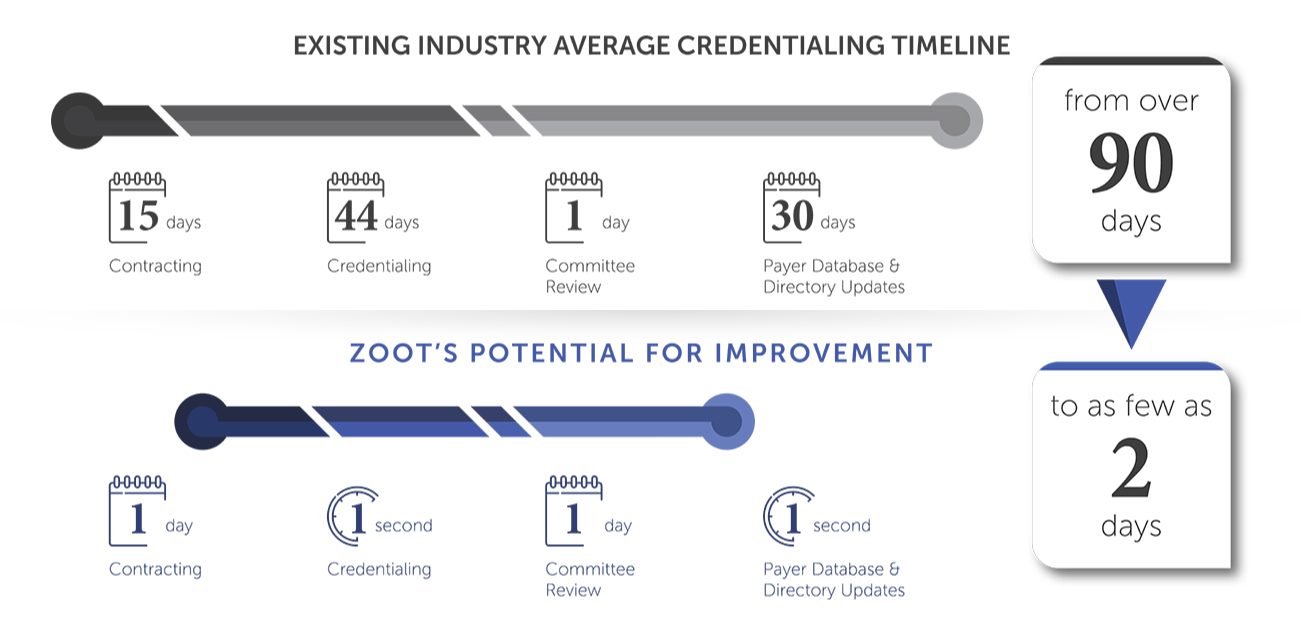
Healthcare organizations are faced with a multitude of challenges and immense pressure when it comes to driving timely revenue, onboarding providers, and streamlining processes. Across the healthcare landscape, the average credentialing timeline is over 90 days long. This current timeline includes approximately 15 days for contracting, 44 days for credentialing, 1 day for committee review, and 30 days to update the payer database and provider directory, during which time patient care and opportunities to generate revenue are delayed.
How would your organization stand to benefit if that 90-day timeline was reduced to as few as two days?
Table of Contents
What is healthcare credentialing?
Credentialing is the process in which a provider’s professional qualifications are reviewed and verified. These qualifications include, but are not limited to, licensure, certifications, training, insurance, and academic background. Every healthcare provider seeking reimbursement from a payer must go through a credentialing process specific to each payer.
Contracting establishes the contract between the payer and healthcare provider for services rendered. This includes basic provider information, the national provider identifier (NPI) number, license, education and any state regulatory requirements to become an approved provider of a specific health plan or insurer.
Credentialing includes the contracting application agreement and adds liability protection for the payer’s health plan members. This includes providing full background of professional work history as well as previous sanctions and legal actions, state regulatory requirements, education, board certifications, and more. Through this process the payer is verifying to their members that the contracted healthcare provider has met the necessary requirements in terms of licensure, expertise, professional history, and liability.
Credentialing is an extra step above the contracting process, providing liability protection for both the insurer and the insured. Both the contracting and credentialing process are required to be completed and verified before submitting to the payer medical committee for review and approval, and before the provider can practice to the full extent of their license. Talented and highly compensated providers are sitting on the sidelines for months waiting on a decision based on an inefficient, manual and error-prone credentialing process. Meanwhile, these providers either cannot see patients at all, or their credentialed colleagues must take additional time to sign off on all services performed, all while receiving benefits and pay that is not offset by revenue being brought in.
Where do things stand in healthcare credentialing?
According to McKinsey, 8% of a payer’s administrative spend is dedicated to the credentialing process. And, nearly one third of credentialing applications received by payers contain inaccurate or incomplete information.
According to a study from the Council for Affordable Quality Healthcare (CAQH), billions of dollars of administrative costs accumulate because of outdated, manual business transactions that are typical for credentialing. Given the annual volume of these transactions, a minimum of 1.1 million hours of manual administrative work could be saved each week simply by automating the most common healthcare transactions.
On average, a single-provider practice holds twelve contracts with health plans and must maintain an average of 140 data elements per contract. This means that a six-provider practice manages over 10,000 data points, creating a huge administrative burden for providers to report – and health plans to collect – data on any changes.
This administrative burden includes a variety of factors:
- Manual, Repetitive Processes: The current credentialing process requires a credentialing specialist to submit similar information to each insurance provider. The manual nature and redundancy of this task often results in applications being submitted with incomplete or incorrect information. An error from something as simple as mistyping data can result in numerous delays and rework.
- Administrative Inconsistency: With no single industry standard for how the credentialing process must be completed, each insurance company uses their own unique application form and process. An estimated 2-2.5% of provider data changes each month, triggering added iterations of the data management process and creating even more opportunities for error.
- Fragmented Data: During payer enrollment, the provider data gathered is constantly pulled from and verified by a variety of sources including providers, national board records, and other third parties. Because the supporting documents are typically physical copies that are scanned in and sent as attachments, the payer may receive files with illegible or incomplete information, resulting in more delays.
What are the benefits of automated credentialing?
Automation in the healthcare credentialing process offers numerous benefits that lead to enhanced efficiency, accuracy, and a stronger overall workflow.
Here are some key advantages:
- Streamlined Manual Processes: Leverage automation to speed up tasks and enhance accuracy with sophisticated data validation to reduce errors and automatically flag incomplete or missing documents within applications.
- Enhanced Data Management: Automation ensures that all credentialing data is stored in a centralized, easily accessible system, improving data management and making it easier to track, retrieve, and update information as needed.
- Increased Scalability: Automated systems can easily scale to handle increasing volumes of credentialing requests without a corresponding increase in manual labor, making it easier to manage growth and changes in the healthcare landscape.
- Faster Revenue Generation: Create a faster path to provider revenue generation by reducing the time during which they cannot practice to the full extent of their license.
- Improved Communication: Automated systems facilitate better communication between different departments and organizations. Notifications and updates can be sent automatically, keeping all stakeholders informed and reducing bottlenecks.
- Enhanced Efficiency: Optimize organizational and staffing resources, freeing up your team to focus on other high-value initiatives and tasks to move your organization forward.
- Seamless Database Connections: Ensure reliable and up-to-date information by automating connections to NPPPES, DEA/CDS, ABMS, FSMB, OIG, NPDB, and more, without compromising on security and compliance.
Improve outcomes with automated credentialing
Zoot is on a mission to reduce spend, improve health outcomes and streamline healthcare processes by optimizing the credentialing process for healthcare providers and payers.
Zoot’s automated credentialing solution leverages advanced data management to reduce the credentialing timeline from 90 days to a little as two. Achieve timely and accurate vetting and enhance your onboarding process with a custom-tailored solution powered by access to powerful data and workflows. With in-line data validation and primary source verification and system-to-system integration that supports the No Surprises Act mandated provider roster and directory updates, your organization maintains full, unwavering compliance.